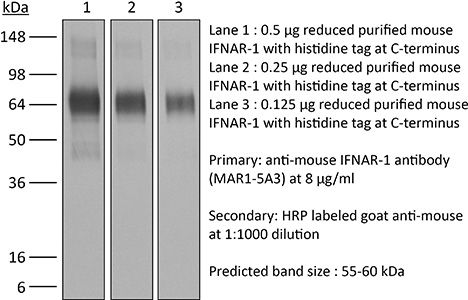
InVivoMAb anti-mouse IFNAR-1
Product Description
Bio X Cell is pleased to also offer MAR1-5A3-CP056. This monoclonal antibody is a recombinant, chimeric version of the original MAR1-5A3 antibody. The variable domain sequences are identical to clone MAR1-5A3, but the constant region has been converted from mouse IgG1 to mouse IgG2a. MAR1-5A3-CP056 also contains Fc silencing mutations rendering it unable to bind to endogenous Fcγ receptors, similar to therapeutic anti-IFNAR-1 antibodies such as Anifrolumab. These mutations prevent Fc-effector functions like antibody-dependent cellular cytotoxicity (ADCC) and complement-dependent cytotoxicity (CDC). The highly controlled sequence and lack of genetic drift in recombinant antibodies provide more reliable and reproducible results over hybridoma derived antibodies.
Specifications
| Isotype | Mouse IgG1, κ |
|---|---|
| Recommended Isotype Control(s) | InVivoMAb mouse IgG1 isotype control, unknown specificity |
| Recommended Dilution Buffer | InVivoPure pH 7.0 Dilution Buffer |
| Conjugation | This product is unconjugated. Conjugation is available via our Antibody Conjugation Services. |
| Immunogen | Extracellular domain of mouse IFNAR-1 |
| Reported Applications |
in vivo IFNAR-1 blockade in vitro IFNAR-1 blockade Western blot Flow Cytometry ELISA |
| Formulation |
PBS, pH 7.0 Contains no stabilizers or preservatives |
| Endotoxin |
≤1EU/mg (≤0.001EU/μg) Determined by LAL assay |
| Purity |
≥95% Determined by SDS-PAGE |
| Sterility | 0.2 µm filtration |
| Production | Purified from cell culture supernatant in an animal-free facility |
| Purification | Protein G |
| RRID | AB_2687723 |
| Molecular Weight | 150 kDa |
| Storage | The antibody solution should be stored at the stock concentration at 4°C. Do not freeze. |
| Need a Custom Formulation? | See All Antibody Customization Options |
Application References
in vitro IFNAR-1 blockade
Hosseini S, Michaelsen-Preusse K, Grigoryan G, Chhatbar C, Kalinke U, Korte M (2020). "Type I Interferon Receptor Signaling in Astrocytes Regulates Hippocampal Synaptic Plasticity and Cognitive Function of the Healthy CNS" Cell Rep 31(7):107666.
PubMed
Type I interferon receptor (IFNAR) signaling is a hallmark of viral control and host protection. Here, we show that, in the hippocampus of healthy IFNAR-deficient mice, synapse number and synaptic plasticity, as well as spatial learning, are impaired. This is also the case for IFN-β-deficient animals. Moreover, antibody-mediated IFNAR blocking acutely interferes with neuronal plasticity, whereas a low-dose application of IFN-β has a positive effect on dendritic spine structure. Interfering with IFNAR signaling in different cell types shows a role for cognitive function and synaptic plasticity specifically mediated by astrocytes. Intriguingly, levels of the astrocytic glutamate-aspartate transporter (GLAST) are reduced significantly upon IFN-β treatment and increase following inhibition of IFNAR signaling. These results indicate that, besides the prominent role for host defense, IFNAR is important for synaptic plasticity as well as cognitive function. Astrocytes are at the center stage of this so-far-unknown signaling cascade.
in vitro IFNAR-1 blockade
Hosseini S, Michaelsen-Preusse K, Grigoryan G, Chhatbar C, Kalinke U, Korte M (2020). "Type I Interferon Receptor Signaling in Astrocytes Regulates Hippocampal Synaptic Plasticity and Cognitive Function of the Healthy CNS" Cell Rep 31(7):107666.
PubMed
Type I interferon receptor (IFNAR) signaling is a hallmark of viral control and host protection. Here, we show that, in the hippocampus of healthy IFNAR-deficient mice, synapse number and synaptic plasticity, as well as spatial learning, are impaired. This is also the case for IFN-β-deficient animals. Moreover, antibody-mediated IFNAR blocking acutely interferes with neuronal plasticity, whereas a low-dose application of IFN-β has a positive effect on dendritic spine structure. Interfering with IFNAR signaling in different cell types shows a role for cognitive function and synaptic plasticity specifically mediated by astrocytes. Intriguingly, levels of the astrocytic glutamate-aspartate transporter (GLAST) are reduced significantly upon IFN-β treatment and increase following inhibition of IFNAR signaling. These results indicate that, besides the prominent role for host defense, IFNAR is important for synaptic plasticity as well as cognitive function. Astrocytes are at the center stage of this so-far-unknown signaling cascade.
in vitro IFNAR-1 blockade
Falahat R, Berglund A, Perez-Villarroel P, Putney RM, Hamaidi I, Kim S, Pilon-Thomas S, Barber GN, Mulé JJ (2023). "Epigenetic state determines the in vivo efficacy of STING agonist therapy" Nat Commun 14(1):1573.
PubMed
While STING-activating agents have shown limited efficacy in early-phase clinical trials, multiple lines of evidence suggest the importance of tumor cell-intrinsic STING function in mediating antitumor immune responses. Although STING signaling is impaired in human melanoma, its restoration through epigenetic reprogramming can augment its antigenicity and T cell recognition. In this study, we show that reversal of methylation silencing of STING in murine melanoma cell lines using a clinically available DNA methylation inhibitor can improve agonist-induced STING activation and type-I IFN induction, which, in tumor-bearing mice, can induce tumor regression through a CD8+ T cell-dependent immune response. These findings not only provide mechanistic insight into how STING signaling dysfunction in tumor cells can contribute to impaired responses to STING agonist therapy, but also suggest that pharmacological restoration of STING signaling through epigenetic reprogramming might improve the therapeutic efficacy of STING agonists.
ELISA
Lomakova YD, Londregan J, Maslanka J, Goldman N, Somerville J, Riggs JE (2019). "PHA eludes macrophage suppression to activate CD8+ T cells" Immunobiology 224(1):94-101.
PubMed
Tumors may include a high proportion of immune modulatory cells and molecules that restrain the anti-cancer response. Activation of T cells to eliminate cancer cells within the immune-suppressive tumor microenvironment remains a challenge. We have shown that C57BL/6 J peritoneal cell culture models features of macrophage-dense tumors as TCR ligation fails to activate T cells unless IFNγ is neutralized or iNOS is inhibited. We tested other forms of T cell activation and found phytohemagglutinin (PHA) distinctive in the ability to markedly expand CD8 T cells in this model. IFNγ or iNOS inhibition was not necessary for this response. PHA triggered less IFNγ production and inhibitory PD-L1 expression than TCR ligation. Macrophages and CD44hi T cells bound PHA. Spleen T cell responses to PHA were markedly enhanced by the addition of peritoneal cells revealing that macrophages enhance T cell expansion. That PHA increases CD8 T cell responses within macrophage-dense culture suggests this mitogen might enhance anti-tumor immunity.
Flow Cytometry
Troegeler A, Mercier I, Cougoule C, Pietretti D, Colom A, Duval C, Vu Manh TP, Capilla F, Poincloux R, Pingris K, Nigou J, Rademann J, Dalod M, Verreck FA, Al Saati T, Lugo-Villarino G, Lepenies B, Hudrisier D, Neyrolles O (2017). "C-type lectin rece
PubMed
Immune response against pathogens is a tightly regulated process that must ensure microbial control while preserving integrity of the infected organs. Tuberculosis (TB) is a paramount example of a chronic infection in which antimicrobial immunity is protective in the vast majority of infected individuals but can become detrimental if not finely tuned. Here, we report that C-type lectin dendritic cell (DC) immunoreceptor (DCIR), a key component in DC homeostasis, is required to modulate lung inflammation and bacterial burden in TB. DCIR is abundantly expressed in pulmonary lesions in Mycobacterium tuberculosis-infected nonhuman primates during both latent and active disease. In mice, we found that DCIR deficiency impairs STAT1-mediated type I IFN signaling in DCs, leading to increased production of IL-12 and increased differentiation of T lymphocytes toward Th1 during infection. As a consequence, DCIR-deficient mice control M. tuberculosis better than WT animals but also develop more inflammation characterized by an increased production of TNF and inducible NOS (iNOS) in the lungs. Altogether, our results reveal a pathway by which a C-type lectin modulates the equilibrium between infection-driven inflammation and pathogen's control through sustaining type I IFN signaling in DCs.
in vitro IFNAR-1 blockade
Hosseini S, Michaelsen-Preusse K, Grigoryan G, Chhatbar C, Kalinke U, Korte M (2020). "Type I Interferon Receptor Signaling in Astrocytes Regulates Hippocampal Synaptic Plasticity and Cognitive Function of the Healthy CNS" Cell Rep 31(7):107666.
PubMed
Type I interferon receptor (IFNAR) signaling is a hallmark of viral control and host protection. Here, we show that, in the hippocampus of healthy IFNAR-deficient mice, synapse number and synaptic plasticity, as well as spatial learning, are impaired. This is also the case for IFN-β-deficient animals. Moreover, antibody-mediated IFNAR blocking acutely interferes with neuronal plasticity, whereas a low-dose application of IFN-β has a positive effect on dendritic spine structure. Interfering with IFNAR signaling in different cell types shows a role for cognitive function and synaptic plasticity specifically mediated by astrocytes. Intriguingly, levels of the astrocytic glutamate-aspartate transporter (GLAST) are reduced significantly upon IFN-β treatment and increase following inhibition of IFNAR signaling. These results indicate that, besides the prominent role for host defense, IFNAR is important for synaptic plasticity as well as cognitive function. Astrocytes are at the center stage of this so-far-unknown signaling cascade.
in vitro IFNAR-1 blockade
Hosseini S, Michaelsen-Preusse K, Grigoryan G, Chhatbar C, Kalinke U, Korte M (2020). "Type I Interferon Receptor Signaling in Astrocytes Regulates Hippocampal Synaptic Plasticity and Cognitive Function of the Healthy CNS" Cell Rep 31(7):107666.
PubMed
Type I interferon receptor (IFNAR) signaling is a hallmark of viral control and host protection. Here, we show that, in the hippocampus of healthy IFNAR-deficient mice, synapse number and synaptic plasticity, as well as spatial learning, are impaired. This is also the case for IFN-β-deficient animals. Moreover, antibody-mediated IFNAR blocking acutely interferes with neuronal plasticity, whereas a low-dose application of IFN-β has a positive effect on dendritic spine structure. Interfering with IFNAR signaling in different cell types shows a role for cognitive function and synaptic plasticity specifically mediated by astrocytes. Intriguingly, levels of the astrocytic glutamate-aspartate transporter (GLAST) are reduced significantly upon IFN-β treatment and increase following inhibition of IFNAR signaling. These results indicate that, besides the prominent role for host defense, IFNAR is important for synaptic plasticity as well as cognitive function. Astrocytes are at the center stage of this so-far-unknown signaling cascade.
Flow Cytometry
Troegeler A, Mercier I, Cougoule C, Pietretti D, Colom A, Duval C, Vu Manh TP, Capilla F, Poincloux R, Pingris K, Nigou J, Rademann J, Dalod M, Verreck FA, Al Saati T, Lugo-Villarino G, Lepenies B, Hudrisier D, Neyrolles O (2017). "C-type lectin rece
PubMed
Immune response against pathogens is a tightly regulated process that must ensure microbial control while preserving integrity of the infected organs. Tuberculosis (TB) is a paramount example of a chronic infection in which antimicrobial immunity is protective in the vast majority of infected individuals but can become detrimental if not finely tuned. Here, we report that C-type lectin dendritic cell (DC) immunoreceptor (DCIR), a key component in DC homeostasis, is required to modulate lung inflammation and bacterial burden in TB. DCIR is abundantly expressed in pulmonary lesions in Mycobacterium tuberculosis-infected nonhuman primates during both latent and active disease. In mice, we found that DCIR deficiency impairs STAT1-mediated type I IFN signaling in DCs, leading to increased production of IL-12 and increased differentiation of T lymphocytes toward Th1 during infection. As a consequence, DCIR-deficient mice control M. tuberculosis better than WT animals but also develop more inflammation characterized by an increased production of TNF and inducible NOS (iNOS) in the lungs. Altogether, our results reveal a pathway by which a C-type lectin modulates the equilibrium between infection-driven inflammation and pathogen's control through sustaining type I IFN signaling in DCs.
ELISA
Lomakova YD, Londregan J, Maslanka J, Goldman N, Somerville J, Riggs JE (2019). "PHA eludes macrophage suppression to activate CD8+ T cells" Immunobiology 224(1):94-101.
PubMed
Tumors may include a high proportion of immune modulatory cells and molecules that restrain the anti-cancer response. Activation of T cells to eliminate cancer cells within the immune-suppressive tumor microenvironment remains a challenge. We have shown that C57BL/6 J peritoneal cell culture models features of macrophage-dense tumors as TCR ligation fails to activate T cells unless IFNγ is neutralized or iNOS is inhibited. We tested other forms of T cell activation and found phytohemagglutinin (PHA) distinctive in the ability to markedly expand CD8 T cells in this model. IFNγ or iNOS inhibition was not necessary for this response. PHA triggered less IFNγ production and inhibitory PD-L1 expression than TCR ligation. Macrophages and CD44hi T cells bound PHA. Spleen T cell responses to PHA were markedly enhanced by the addition of peritoneal cells revealing that macrophages enhance T cell expansion. That PHA increases CD8 T cell responses within macrophage-dense culture suggests this mitogen might enhance anti-tumor immunity.
in vitro IFNAR-1 blockade
Falahat R, Berglund A, Perez-Villarroel P, Putney RM, Hamaidi I, Kim S, Pilon-Thomas S, Barber GN, Mulé JJ (2023). "Epigenetic state determines the in vivo efficacy of STING agonist therapy" Nat Commun 14(1):1573.
PubMed
While STING-activating agents have shown limited efficacy in early-phase clinical trials, multiple lines of evidence suggest the importance of tumor cell-intrinsic STING function in mediating antitumor immune responses. Although STING signaling is impaired in human melanoma, its restoration through epigenetic reprogramming can augment its antigenicity and T cell recognition. In this study, we show that reversal of methylation silencing of STING in murine melanoma cell lines using a clinically available DNA methylation inhibitor can improve agonist-induced STING activation and type-I IFN induction, which, in tumor-bearing mice, can induce tumor regression through a CD8+ T cell-dependent immune response. These findings not only provide mechanistic insight into how STING signaling dysfunction in tumor cells can contribute to impaired responses to STING agonist therapy, but also suggest that pharmacological restoration of STING signaling through epigenetic reprogramming might improve the therapeutic efficacy of STING agonists.
in vitro IFNAR-1 blockade
Falahat R, Berglund A, Perez-Villarroel P, Putney RM, Hamaidi I, Kim S, Pilon-Thomas S, Barber GN, Mulé JJ (2023). "Epigenetic state determines the in vivo efficacy of STING agonist therapy" Nat Commun 14(1):1573.
PubMed
While STING-activating agents have shown limited efficacy in early-phase clinical trials, multiple lines of evidence suggest the importance of tumor cell-intrinsic STING function in mediating antitumor immune responses. Although STING signaling is impaired in human melanoma, its restoration through epigenetic reprogramming can augment its antigenicity and T cell recognition. In this study, we show that reversal of methylation silencing of STING in murine melanoma cell lines using a clinically available DNA methylation inhibitor can improve agonist-induced STING activation and type-I IFN induction, which, in tumor-bearing mice, can induce tumor regression through a CD8+ T cell-dependent immune response. These findings not only provide mechanistic insight into how STING signaling dysfunction in tumor cells can contribute to impaired responses to STING agonist therapy, but also suggest that pharmacological restoration of STING signaling through epigenetic reprogramming might improve the therapeutic efficacy of STING agonists.
Fc receptor blocking
in vivo CD47 blockade
in vivo IFNAR-1 blockade
in vivo CSF1 neutralization
Flow Cytometry
Liu, X., et al (2015). "CD47 blockade triggers T cell-mediated destruction of immunogenic tumors" Nat Med 21(10): 1209-1215.
PubMed
Macrophage phagocytosis of tumor cells mediated by CD47-specific blocking antibodies has been proposed to be the major effector mechanism in xenograft models. Here, using syngeneic immunocompetent mouse tumor models, we reveal that the therapeutic effects of CD47 blockade depend on dendritic cell but not macrophage cross-priming of T cell responses. The therapeutic effects of anti-CD47 antibody therapy were abrogated in T cell-deficient mice. In addition, the antitumor effects of CD47 blockade required expression of the cytosolic DNA sensor STING, but neither MyD88 nor TRIF, in CD11c(+) cells, suggesting that cytosolic sensing of DNA from tumor cells is enhanced by anti-CD47 treatment, further bridging the innate and adaptive responses. Notably, the timing of administration of standard chemotherapy markedly impacted the induction of antitumor T cell responses by CD47 blockade. Together, our findings indicate that CD47 blockade drives T cell-mediated elimination of immunogenic tumors.
Fc receptor blocking
in vivo CD47 blockade
in vivo IFNAR-1 blockade
in vivo CSF1 neutralization
Flow Cytometry
Liu, X., et al (2015). "CD47 blockade triggers T cell-mediated destruction of immunogenic tumors" Nat Med 21(10): 1209-1215.
PubMed
Macrophage phagocytosis of tumor cells mediated by CD47-specific blocking antibodies has been proposed to be the major effector mechanism in xenograft models. Here, using syngeneic immunocompetent mouse tumor models, we reveal that the therapeutic effects of CD47 blockade depend on dendritic cell but not macrophage cross-priming of T cell responses. The therapeutic effects of anti-CD47 antibody therapy were abrogated in T cell-deficient mice. In addition, the antitumor effects of CD47 blockade required expression of the cytosolic DNA sensor STING, but neither MyD88 nor TRIF, in CD11c(+) cells, suggesting that cytosolic sensing of DNA from tumor cells is enhanced by anti-CD47 treatment, further bridging the innate and adaptive responses. Notably, the timing of administration of standard chemotherapy markedly impacted the induction of antitumor T cell responses by CD47 blockade. Together, our findings indicate that CD47 blockade drives T cell-mediated elimination of immunogenic tumors.
in vivo IFNAR-1 blockade
Stock, A. T., et al (2014). "Type I IFN suppresses Cxcr2 driven neutrophil recruitment into the sensory ganglia during viral infection" J Exp Med 211(5): 751-759.
PubMed
Infection induces the expression of inflammatory chemokines that recruit immune cells to the site of inflammation. Whereas tissues such as the intestine and skin express unique chemokines during homeostasis, whether different tissues express distinct chemokine profiles during inflammation remains unclear. With this in mind, we performed a comprehensive screen of the chemokines expressed by two tissues (skin and sensory ganglia) infected with a common viral pathogen (herpes simplex virus type 1). After infection, the skin and ganglia showed marked differences in their expression of the family of Cxcr2 chemokine ligands. Specifically, Cxcl1/2/3, which in turn controlled neutrophil recruitment, was up-regulated in the skin but absent from the ganglia. Within the ganglia, Cxcl2 expression and subsequent neutrophil recruitment was inhibited by type I interferon (IFN). Using a combination of bone marrow chimeras and intracellular chemokine staining, we show that type I IFN acted by directly suppressing Cxcl2 expression by monocytes, abrogating their ability to recruit neutrophils to the ganglia. Overall, our findings describe a novel role for IFN in the direct, and selective, inhibition of Cxcr2 chemokine ligands, which results in the inhibition of neutrophil recruitment to neuronal tissue.
in vivo IFNAR-1 blockade
Ma, Y., et al (2014). "Borrelia burgdorferi arthritis-associated locus Bbaa1 regulates Lyme arthritis and K/BxN serum transfer arthritis through intrinsic control of type I IFN production" J Immunol 193(12): 6050-6060.
PubMed
Localized upregulation of type I IFN was previously implicated in development of Borrelia burgdorferi-induced arthritis in C3H mice, and was remarkable due to its absence in the mildly arthritic C57BL/6 (B6) mice. Independently, forward genetics analysis identified a quantitative trait locus on Chr4, termed B. burgdorferi-associated locus 1 (Bbaa1), that regulates Lyme arthritis severity and includes the 15 type I IFN genes. Involvement of Bbaa1 in arthritis development was confirmed in B6 mice congenic for the C3H allele of Bbaa1 (B6.C3-Bbaa1), which developed more severe Lyme arthritis and K/BxN model of rheumatoid arthritis (RA) than did parental B6 mice. Administration of a type I IFN receptor blocking mAb reduced the severity of both Lyme arthritis and RA in B6.C3-Bbaa1 mice, formally linking genetic elements within Bbaa1 to pathological production of type I IFN. Bone marrow-derived macrophages from Bbaa1 congenic mice implicated this locus as a regulator of type I IFN induction and downstream target gene expression. Bbaa1-mediated regulation of IFN-inducible genes was upstream of IFN receptor-dependent amplification; however, the overall magnitude of the response was dependent on autocrine/paracrine responses to IFN-beta. In addition, the Bbaa1 locus modulated the functional phenotype ascribed to bone marrow-derived macrophages: the B6 allele promoted expression of M2 markers, whereas the C3H allele promoted induction of M1 responses. This report identifies a genetic locus physically and functionally linked to type I IFN that contributes to the pathogenesis of both Lyme and RA.
in vivo IFNAR-1 blockade
Calame, D. G., et al (2014). "The C5a anaphylatoxin receptor (C5aR1) protects against Listeria monocytogenes infection by inhibiting type 1 IFN expression" J Immunol 193(10): 5099-5107.
PubMed
Listeria monocytogenes is a major cause of mortality resulting from food poisoning in the United States. In mice, C5 has been genetically linked to host resistance to listeriosis. Despite this genetic association, it remains poorly understood how C5 and its activation products, C5a and C5b, confer host protection to this Gram-positive intracellular bacterium. In this article, we show in a systemic infection model that the major receptor for C5a, C5aR1, is required for a normal robust host immune response against L. monocytogenes. In comparison with wild-type mice, C5aR1(-/-) mice had reduced survival and increased bacterial burden in their livers and spleens. Infected C5aR1(-/-) mice exhibited a dramatic reduction in all major subsets of splenocytes, which was associated with elevated caspase-3 activity and increased TUNEL staining. Because type 1 IFN has been reported to impede the host response to L. monocytogenes through the promotion of splenocyte death, we examined the effect of C5aR1 on type 1 IFN expression in vivo. Indeed, serum levels of IFN-alpha and IFN-beta were significantly elevated in L. monocytogenes-infected C5aR1(-/-) mice. Similarly, the expression of TRAIL, a type 1 IFN target gene and a proapoptotic factor, was elevated in NK cells isolated from infected C5aR1(-/-) mice. Treatment of C5aR1(-/-) mice with a type 1 IFNR blocking Ab resulted in near-complete rescue of L. monocytogenes-induced mortality. Thus, these findings reveal a critical role for C5aR1 in host defense against L. monocytogenes through the suppression of type 1 IFN expression.
in vitro TNFα neutralization
in vivo IFNAR-1 blockade
Beug, S. T., et al (2014). "Smac mimetics and innate immune stimuli synergize to promote tumor death" Nat Biotechnol 32(2): 182-190.
PubMed
Smac mimetic compounds (SMC), a class of drugs that sensitize cells to apoptosis by counteracting the activity of inhibitor of apoptosis (IAP) proteins, have proven safe in phase 1 clinical trials in cancer patients. However, because SMCs act by enabling transduction of pro-apoptotic signals, SMC monotherapy may be efficacious only in the subset of patients whose tumors produce large quantities of death-inducing proteins such as inflammatory cytokines. Therefore, we reasoned that SMCs would synergize with agents that stimulate a potent yet safe “cytokine storm.” Here we show that oncolytic viruses and adjuvants such as poly(I:C) and CpG induce bystander death of cancer cells treated with SMCs that is mediated by interferon beta (IFN-beta), tumor necrosis factor alpha (TNF-alpha) and/or TNF-related apoptosis-inducing ligand (TRAIL). This combinatorial treatment resulted in tumor regression and extended survival in two mouse models of cancer. As these and other adjuvants have been proven safe in clinical trials, it may be worthwhile to explore their clinical efficacy in combination with SMCs.
in vivo IFNAR-1 blockade
Macal, M., et al (2018). "Self-Renewal and Toll-like Receptor Signaling Sustain Exhausted Plasmacytoid Dendritic Cells during Chronic Viral Infection" Immunity 48(4): 730-744 e735.
PubMed
Although characterization of T cell exhaustion has unlocked powerful immunotherapies, the mechanisms sustaining adaptations of short-lived innate cells to chronic inflammatory settings remain unknown. During murine chronic viral infection, we found that concerted events in bone marrow and spleen mediated by type I interferon (IFN-I) and Toll-like receptor 7 (TLR7) maintained a pool of functionally exhausted plasmacytoid dendritic cells (pDCs). In the bone marrow, IFN-I compromised the number and the developmental capacity of pDC progenitors, which generated dysfunctional pDCs. Concurrently, exhausted pDCs in the periphery were maintained by self-renewal via IFN-I- and TLR7-induced proliferation of CD4(-) subsets. On the other hand, pDC functional loss was mediated by TLR7, leading to compromised IFN-I production and resistance to secondary infection. These findings unveil the mechanisms sustaining a self-perpetuating pool of functionally exhausted pDCs and provide a framework for deciphering long-term exhaustion of other short-lived innate cells during chronic inflammation.
in vitro IFNAR-1 blockade
Schliehe, C., et al (2015). "The methyltransferase Setdb2 mediates virus-induced susceptibility to bacterial superinfection" Nat Immunol 16(1): 67-74.
PubMed
Immune responses are tightly regulated to ensure efficient pathogen clearance while avoiding tissue damage. Here we report that Setdb2 was the only protein lysine methyltransferase induced during infection with influenza virus. Setdb2 expression depended on signaling via type I interferons, and Setdb2 repressed expression of the gene encoding the neutrophil attractant CXCL1 and other genes that are targets of the transcription factor NF-kappaB. This coincided with occupancy by Setdb2 at the Cxcl1 promoter, which in the absence of Setdb2 displayed diminished trimethylation of histone H3 Lys9 (H3K9me3). Mice with a hypomorphic gene-trap construct of Setdb2 exhibited increased infiltration of neutrophils during sterile lung inflammation and were less sensitive to bacterial superinfection after infection with influenza virus. This suggested that a Setdb2-mediated regulatory crosstalk between the type I interferons and NF-kappaB pathways represents an important mechanism for virus-induced susceptibility to bacterial superinfection.
in vivo IFNAR-1 blockade
in vivo CXCR3 neutralization
Yang, H., et al (2015). "STAT3 Inhibition Enhances the Therapeutic Efficacy of Immunogenic Chemotherapy by Stimulating Type 1 Interferon Production by Cancer Cells" Cancer Res 75(18): 3812-3822.
PubMed
STAT3 is an oncogenic transcription factor with potent immunosuppressive functions. We found that pharmacologic inhibition of STAT3 or its selective knockout in cancer cells improved the tumor growth-inhibitory efficacy of anthracycline-based chemotherapies. This combined effect of STAT3 inhibition/depletion and anthracyclines was only found in tumors growing on immunocompetent (not in immunodeficient) mice. As compared with Stat3-sufficient control tumors, Stat3(-/-) cancer cells exhibited an increased infiltration by dendritic cells and cytotoxic T lymphocytes after chemotherapy. Anthracyclines are known to induce several stress pathways that enhance the immunogenicity of dying and dead cancer cells, thereby stimulating a dendritic cell-dependent and T lymphocyte-mediated anticancer immune response. Among these therapy-relevant stress pathways, Stat3(-/-) cancer cells manifested one significant improvement, namely an increase in the expression of multiple type-1 interferon-responsive genes, including that of the chemokines Cxcl9 and Cxcl10. This enhanced type-1 interferon response could be suppressed by reintroducing wild-type Stat3 (but not a transactivation-deficient mutant Stat3(Y705F)) into the tumor cells. This maneuver also abolished the improved chemotherapeutic response of Stat3(-/-) cancers. Finally, the neutralization of the common type-1 interferon receptor or that of the chemokine receptor CXCR3 (which binds CXCL9 and CXCL10) abolished the difference in the chemotherapeutic response between Stat3(-/-) and control tumors. Altogether, these results suggest that STAT3 inhibitors may improve the outcome of chemotherapy by enhancing the type-1 interferon response of cancer cells.
in vivo IFNAR-1 blockade
Calame, D. G., et al (2014). "The C5a anaphylatoxin receptor (C5aR1) protects against Listeria monocytogenes infection by inhibiting type 1 IFN expression" J Immunol 193(10): 5099-5107.
PubMed
Listeria monocytogenes is a major cause of mortality resulting from food poisoning in the United States. In mice, C5 has been genetically linked to host resistance to listeriosis. Despite this genetic association, it remains poorly understood how C5 and its activation products, C5a and C5b, confer host protection to this Gram-positive intracellular bacterium. In this article, we show in a systemic infection model that the major receptor for C5a, C5aR1, is required for a normal robust host immune response against L. monocytogenes. In comparison with wild-type mice, C5aR1(-/-) mice had reduced survival and increased bacterial burden in their livers and spleens. Infected C5aR1(-/-) mice exhibited a dramatic reduction in all major subsets of splenocytes, which was associated with elevated caspase-3 activity and increased TUNEL staining. Because type 1 IFN has been reported to impede the host response to L. monocytogenes through the promotion of splenocyte death, we examined the effect of C5aR1 on type 1 IFN expression in vivo. Indeed, serum levels of IFN-alpha and IFN-beta were significantly elevated in L. monocytogenes-infected C5aR1(-/-) mice. Similarly, the expression of TRAIL, a type 1 IFN target gene and a proapoptotic factor, was elevated in NK cells isolated from infected C5aR1(-/-) mice. Treatment of C5aR1(-/-) mice with a type 1 IFNR blocking Ab resulted in near-complete rescue of L. monocytogenes-induced mortality. Thus, these findings reveal a critical role for C5aR1 in host defense against L. monocytogenes through the suppression of type 1 IFN expression.
in vivo IFNAR-1 blockade
Ma, Y., et al (2014). "Borrelia burgdorferi arthritis-associated locus Bbaa1 regulates Lyme arthritis and K/BxN serum transfer arthritis through intrinsic control of type I IFN production" J Immunol 193(12): 6050-6060.
PubMed
Localized upregulation of type I IFN was previously implicated in development of Borrelia burgdorferi-induced arthritis in C3H mice, and was remarkable due to its absence in the mildly arthritic C57BL/6 (B6) mice. Independently, forward genetics analysis identified a quantitative trait locus on Chr4, termed B. burgdorferi-associated locus 1 (Bbaa1), that regulates Lyme arthritis severity and includes the 15 type I IFN genes. Involvement of Bbaa1 in arthritis development was confirmed in B6 mice congenic for the C3H allele of Bbaa1 (B6.C3-Bbaa1), which developed more severe Lyme arthritis and K/BxN model of rheumatoid arthritis (RA) than did parental B6 mice. Administration of a type I IFN receptor blocking mAb reduced the severity of both Lyme arthritis and RA in B6.C3-Bbaa1 mice, formally linking genetic elements within Bbaa1 to pathological production of type I IFN. Bone marrow-derived macrophages from Bbaa1 congenic mice implicated this locus as a regulator of type I IFN induction and downstream target gene expression. Bbaa1-mediated regulation of IFN-inducible genes was upstream of IFN receptor-dependent amplification; however, the overall magnitude of the response was dependent on autocrine/paracrine responses to IFN-beta. In addition, the Bbaa1 locus modulated the functional phenotype ascribed to bone marrow-derived macrophages: the B6 allele promoted expression of M2 markers, whereas the C3H allele promoted induction of M1 responses. This report identifies a genetic locus physically and functionally linked to type I IFN that contributes to the pathogenesis of both Lyme and RA.
in vivo IFNAR-1 blockade
Stock, A. T., et al (2014). "Type I IFN suppresses Cxcr2 driven neutrophil recruitment into the sensory ganglia during viral infection" J Exp Med 211(5): 751-759.
PubMed
Infection induces the expression of inflammatory chemokines that recruit immune cells to the site of inflammation. Whereas tissues such as the intestine and skin express unique chemokines during homeostasis, whether different tissues express distinct chemokine profiles during inflammation remains unclear. With this in mind, we performed a comprehensive screen of the chemokines expressed by two tissues (skin and sensory ganglia) infected with a common viral pathogen (herpes simplex virus type 1). After infection, the skin and ganglia showed marked differences in their expression of the family of Cxcr2 chemokine ligands. Specifically, Cxcl1/2/3, which in turn controlled neutrophil recruitment, was up-regulated in the skin but absent from the ganglia. Within the ganglia, Cxcl2 expression and subsequent neutrophil recruitment was inhibited by type I interferon (IFN). Using a combination of bone marrow chimeras and intracellular chemokine staining, we show that type I IFN acted by directly suppressing Cxcl2 expression by monocytes, abrogating their ability to recruit neutrophils to the ganglia. Overall, our findings describe a novel role for IFN in the direct, and selective, inhibition of Cxcr2 chemokine ligands, which results in the inhibition of neutrophil recruitment to neuronal tissue.
in vivo IFNAR-1 blockade
in vivo CXCR3 neutralization
Yang, H., et al (2015). "STAT3 Inhibition Enhances the Therapeutic Efficacy of Immunogenic Chemotherapy by Stimulating Type 1 Interferon Production by Cancer Cells" Cancer Res 75(18): 3812-3822.
PubMed
STAT3 is an oncogenic transcription factor with potent immunosuppressive functions. We found that pharmacologic inhibition of STAT3 or its selective knockout in cancer cells improved the tumor growth-inhibitory efficacy of anthracycline-based chemotherapies. This combined effect of STAT3 inhibition/depletion and anthracyclines was only found in tumors growing on immunocompetent (not in immunodeficient) mice. As compared with Stat3-sufficient control tumors, Stat3(-/-) cancer cells exhibited an increased infiltration by dendritic cells and cytotoxic T lymphocytes after chemotherapy. Anthracyclines are known to induce several stress pathways that enhance the immunogenicity of dying and dead cancer cells, thereby stimulating a dendritic cell-dependent and T lymphocyte-mediated anticancer immune response. Among these therapy-relevant stress pathways, Stat3(-/-) cancer cells manifested one significant improvement, namely an increase in the expression of multiple type-1 interferon-responsive genes, including that of the chemokines Cxcl9 and Cxcl10. This enhanced type-1 interferon response could be suppressed by reintroducing wild-type Stat3 (but not a transactivation-deficient mutant Stat3(Y705F)) into the tumor cells. This maneuver also abolished the improved chemotherapeutic response of Stat3(-/-) cancers. Finally, the neutralization of the common type-1 interferon receptor or that of the chemokine receptor CXCR3 (which binds CXCL9 and CXCL10) abolished the difference in the chemotherapeutic response between Stat3(-/-) and control tumors. Altogether, these results suggest that STAT3 inhibitors may improve the outcome of chemotherapy by enhancing the type-1 interferon response of cancer cells.
in vitro IFNAR-1 blockade
Schliehe, C., et al (2015). "The methyltransferase Setdb2 mediates virus-induced susceptibility to bacterial superinfection" Nat Immunol 16(1): 67-74.
PubMed
Immune responses are tightly regulated to ensure efficient pathogen clearance while avoiding tissue damage. Here we report that Setdb2 was the only protein lysine methyltransferase induced during infection with influenza virus. Setdb2 expression depended on signaling via type I interferons, and Setdb2 repressed expression of the gene encoding the neutrophil attractant CXCL1 and other genes that are targets of the transcription factor NF-kappaB. This coincided with occupancy by Setdb2 at the Cxcl1 promoter, which in the absence of Setdb2 displayed diminished trimethylation of histone H3 Lys9 (H3K9me3). Mice with a hypomorphic gene-trap construct of Setdb2 exhibited increased infiltration of neutrophils during sterile lung inflammation and were less sensitive to bacterial superinfection after infection with influenza virus. This suggested that a Setdb2-mediated regulatory crosstalk between the type I interferons and NF-kappaB pathways represents an important mechanism for virus-induced susceptibility to bacterial superinfection.
in vivo IFNAR-1 blockade
Macal, M., et al (2018). "Self-Renewal and Toll-like Receptor Signaling Sustain Exhausted Plasmacytoid Dendritic Cells during Chronic Viral Infection" Immunity 48(4): 730-744 e735.
PubMed
Although characterization of T cell exhaustion has unlocked powerful immunotherapies, the mechanisms sustaining adaptations of short-lived innate cells to chronic inflammatory settings remain unknown. During murine chronic viral infection, we found that concerted events in bone marrow and spleen mediated by type I interferon (IFN-I) and Toll-like receptor 7 (TLR7) maintained a pool of functionally exhausted plasmacytoid dendritic cells (pDCs). In the bone marrow, IFN-I compromised the number and the developmental capacity of pDC progenitors, which generated dysfunctional pDCs. Concurrently, exhausted pDCs in the periphery were maintained by self-renewal via IFN-I- and TLR7-induced proliferation of CD4(-) subsets. On the other hand, pDC functional loss was mediated by TLR7, leading to compromised IFN-I production and resistance to secondary infection. These findings unveil the mechanisms sustaining a self-perpetuating pool of functionally exhausted pDCs and provide a framework for deciphering long-term exhaustion of other short-lived innate cells during chronic inflammation.
in vitro TNFα neutralization
in vivo IFNAR-1 blockade
Beug, S. T., et al (2014). "Smac mimetics and innate immune stimuli synergize to promote tumor death" Nat Biotechnol 32(2): 182-190.
PubMed
Smac mimetic compounds (SMC), a class of drugs that sensitize cells to apoptosis by counteracting the activity of inhibitor of apoptosis (IAP) proteins, have proven safe in phase 1 clinical trials in cancer patients. However, because SMCs act by enabling transduction of pro-apoptotic signals, SMC monotherapy may be efficacious only in the subset of patients whose tumors produce large quantities of death-inducing proteins such as inflammatory cytokines. Therefore, we reasoned that SMCs would synergize with agents that stimulate a potent yet safe “cytokine storm.” Here we show that oncolytic viruses and adjuvants such as poly(I:C) and CpG induce bystander death of cancer cells treated with SMCs that is mediated by interferon beta (IFN-beta), tumor necrosis factor alpha (TNF-alpha) and/or TNF-related apoptosis-inducing ligand (TRAIL). This combinatorial treatment resulted in tumor regression and extended survival in two mouse models of cancer. As these and other adjuvants have been proven safe in clinical trials, it may be worthwhile to explore their clinical efficacy in combination with SMCs.
in vivo CTLA-4 neutralization
in vivo IFNAR-1 blockade
in vivo blocking of OX40/OX40L signaling
in vivo 4-1BBL blockade
Welten, S. P., et al (2015). "The viral context instructs the redundancy of costimulatory pathways in driving CD8(+) T cell expansion" Elife 4. doi : 10.7554/eLife.07486.
PubMed
Signals delivered by costimulatory molecules are implicated in driving T cell expansion. The requirements for these signals, however, vary from dispensable to essential in different infections. We examined the underlying mechanisms of this differential T cell costimulation dependence and found that the viral context determined the dependence on CD28/B7-mediated costimulation for expansion of naive and memory CD8(+) T cells, indicating that the requirement for costimulatory signals is not imprinted. Notably, related to the high-level costimulatory molecule expression induced by lymphocytic choriomeningitis virus (LCMV), CD28/B7-mediated costimulation was dispensable for accumulation of LCMV-specific CD8(+) T cells because of redundancy with the costimulatory pathways induced by TNF receptor family members (i.e., CD27, OX40, and 4-1BB). Type I IFN signaling in viral-specific CD8(+) T cells is slightly redundant with costimulatory signals. These results highlight that pathogen-specific conditions differentially and uniquely dictate the utilization of costimulatory pathways allowing shaping of effector and memory antigen-specific CD8(+) T cell responses.
in vivo CTLA-4 neutralization
in vivo IFNAR-1 blockade
in vivo blocking of OX40/OX40L signaling
in vivo 4-1BBL blockade
Welten, S. P., et al (2015). "The viral context instructs the redundancy of costimulatory pathways in driving CD8(+) T cell expansion" Elife 4. doi : 10.7554/eLife.07486.
PubMed
Signals delivered by costimulatory molecules are implicated in driving T cell expansion. The requirements for these signals, however, vary from dispensable to essential in different infections. We examined the underlying mechanisms of this differential T cell costimulation dependence and found that the viral context determined the dependence on CD28/B7-mediated costimulation for expansion of naive and memory CD8(+) T cells, indicating that the requirement for costimulatory signals is not imprinted. Notably, related to the high-level costimulatory molecule expression induced by lymphocytic choriomeningitis virus (LCMV), CD28/B7-mediated costimulation was dispensable for accumulation of LCMV-specific CD8(+) T cells because of redundancy with the costimulatory pathways induced by TNF receptor family members (i.e., CD27, OX40, and 4-1BB). Type I IFN signaling in viral-specific CD8(+) T cells is slightly redundant with costimulatory signals. These results highlight that pathogen-specific conditions differentially and uniquely dictate the utilization of costimulatory pathways allowing shaping of effector and memory antigen-specific CD8(+) T cell responses.
in vitro IFNAR-1 blockade
Hosseini S, Michaelsen-Preusse K, Grigoryan G, Chhatbar C, Kalinke U, Korte M (2020). "Type I Interferon Receptor Signaling in Astrocytes Regulates Hippocampal Synaptic Plasticity and Cognitive Function of the Healthy CNS" Cell Rep 31(7):107666.
PubMed
Type I interferon receptor (IFNAR) signaling is a hallmark of viral control and host protection. Here, we show that, in the hippocampus of healthy IFNAR-deficient mice, synapse number and synaptic plasticity, as well as spatial learning, are impaired. This is also the case for IFN-β-deficient animals. Moreover, antibody-mediated IFNAR blocking acutely interferes with neuronal plasticity, whereas a low-dose application of IFN-β has a positive effect on dendritic spine structure. Interfering with IFNAR signaling in different cell types shows a role for cognitive function and synaptic plasticity specifically mediated by astrocytes. Intriguingly, levels of the astrocytic glutamate-aspartate transporter (GLAST) are reduced significantly upon IFN-β treatment and increase following inhibition of IFNAR signaling. These results indicate that, besides the prominent role for host defense, IFNAR is important for synaptic plasticity as well as cognitive function. Astrocytes are at the center stage of this so-far-unknown signaling cascade.
in vitro IFNAR-1 blockade
Hosseini S, Michaelsen-Preusse K, Grigoryan G, Chhatbar C, Kalinke U, Korte M (2020). "Type I Interferon Receptor Signaling in Astrocytes Regulates Hippocampal Synaptic Plasticity and Cognitive Function of the Healthy CNS" Cell Rep 31(7):107666.
PubMed
Type I interferon receptor (IFNAR) signaling is a hallmark of viral control and host protection. Here, we show that, in the hippocampus of healthy IFNAR-deficient mice, synapse number and synaptic plasticity, as well as spatial learning, are impaired. This is also the case for IFN-β-deficient animals. Moreover, antibody-mediated IFNAR blocking acutely interferes with neuronal plasticity, whereas a low-dose application of IFN-β has a positive effect on dendritic spine structure. Interfering with IFNAR signaling in different cell types shows a role for cognitive function and synaptic plasticity specifically mediated by astrocytes. Intriguingly, levels of the astrocytic glutamate-aspartate transporter (GLAST) are reduced significantly upon IFN-β treatment and increase following inhibition of IFNAR signaling. These results indicate that, besides the prominent role for host defense, IFNAR is important for synaptic plasticity as well as cognitive function. Astrocytes are at the center stage of this so-far-unknown signaling cascade.
ELISA
Lomakova YD, Londregan J, Maslanka J, Goldman N, Somerville J, Riggs JE (2019). "PHA eludes macrophage suppression to activate CD8+ T cells" Immunobiology 224(1):94-101.
PubMed
Tumors may include a high proportion of immune modulatory cells and molecules that restrain the anti-cancer response. Activation of T cells to eliminate cancer cells within the immune-suppressive tumor microenvironment remains a challenge. We have shown that C57BL/6 J peritoneal cell culture models features of macrophage-dense tumors as TCR ligation fails to activate T cells unless IFNγ is neutralized or iNOS is inhibited. We tested other forms of T cell activation and found phytohemagglutinin (PHA) distinctive in the ability to markedly expand CD8 T cells in this model. IFNγ or iNOS inhibition was not necessary for this response. PHA triggered less IFNγ production and inhibitory PD-L1 expression than TCR ligation. Macrophages and CD44hi T cells bound PHA. Spleen T cell responses to PHA were markedly enhanced by the addition of peritoneal cells revealing that macrophages enhance T cell expansion. That PHA increases CD8 T cell responses within macrophage-dense culture suggests this mitogen might enhance anti-tumor immunity.
in vivo IFNAR-1 blockade
Macal, M., et al (2018). "Self-Renewal and Toll-like Receptor Signaling Sustain Exhausted Plasmacytoid Dendritic Cells during Chronic Viral Infection" Immunity 48(4): 730-744 e735.
PubMed
Although characterization of T cell exhaustion has unlocked powerful immunotherapies, the mechanisms sustaining adaptations of short-lived innate cells to chronic inflammatory settings remain unknown. During murine chronic viral infection, we found that concerted events in bone marrow and spleen mediated by type I interferon (IFN-I) and Toll-like receptor 7 (TLR7) maintained a pool of functionally exhausted plasmacytoid dendritic cells (pDCs). In the bone marrow, IFN-I compromised the number and the developmental capacity of pDC progenitors, which generated dysfunctional pDCs. Concurrently, exhausted pDCs in the periphery were maintained by self-renewal via IFN-I- and TLR7-induced proliferation of CD4(-) subsets. On the other hand, pDC functional loss was mediated by TLR7, leading to compromised IFN-I production and resistance to secondary infection. These findings unveil the mechanisms sustaining a self-perpetuating pool of functionally exhausted pDCs and provide a framework for deciphering long-term exhaustion of other short-lived innate cells during chronic inflammation.
Flow Cytometry
Troegeler A, Mercier I, Cougoule C, Pietretti D, Colom A, Duval C, Vu Manh TP, Capilla F, Poincloux R, Pingris K, Nigou J, Rademann J, Dalod M, Verreck FA, Al Saati T, Lugo-Villarino G, Lepenies B, Hudrisier D, Neyrolles O (2017). "C-type lectin rece
PubMed
Immune response against pathogens is a tightly regulated process that must ensure microbial control while preserving integrity of the infected organs. Tuberculosis (TB) is a paramount example of a chronic infection in which antimicrobial immunity is protective in the vast majority of infected individuals but can become detrimental if not finely tuned. Here, we report that C-type lectin dendritic cell (DC) immunoreceptor (DCIR), a key component in DC homeostasis, is required to modulate lung inflammation and bacterial burden in TB. DCIR is abundantly expressed in pulmonary lesions in Mycobacterium tuberculosis-infected nonhuman primates during both latent and active disease. In mice, we found that DCIR deficiency impairs STAT1-mediated type I IFN signaling in DCs, leading to increased production of IL-12 and increased differentiation of T lymphocytes toward Th1 during infection. As a consequence, DCIR-deficient mice control M. tuberculosis better than WT animals but also develop more inflammation characterized by an increased production of TNF and inducible NOS (iNOS) in the lungs. Altogether, our results reveal a pathway by which a C-type lectin modulates the equilibrium between infection-driven inflammation and pathogen's control through sustaining type I IFN signaling in DCs.
in vivo IFNAR-1 blockade
Liu, X., et al (2015). "CD47 blockade triggers T cell-mediated destruction of immunogenic tumors" Nat Med 21(10): 1209-1215.
PubMed
Macrophage phagocytosis of tumor cells mediated by CD47-specific blocking antibodies has been proposed to be the major effector mechanism in xenograft models. Here, using syngeneic immunocompetent mouse tumor models, we reveal that the therapeutic effects of CD47 blockade depend on dendritic cell but not macrophage cross-priming of T cell responses. The therapeutic effects of anti-CD47 antibody therapy were abrogated in T cell-deficient mice. In addition, the antitumor effects of CD47 blockade required expression of the cytosolic DNA sensor STING, but neither MyD88 nor TRIF, in CD11c(+) cells, suggesting that cytosolic sensing of DNA from tumor cells is enhanced by anti-CD47 treatment, further bridging the innate and adaptive responses. Notably, the timing of administration of standard chemotherapy markedly impacted the induction of antitumor T cell responses by CD47 blockade. Together, our findings indicate that CD47 blockade drives T cell-mediated elimination of immunogenic tumors.
in vitro IFNAR-1 blockade
Schliehe, C., et al (2015). "The methyltransferase Setdb2 mediates virus-induced susceptibility to bacterial superinfection" Nat Immunol 16(1): 67-74.
PubMed
Immune responses are tightly regulated to ensure efficient pathogen clearance while avoiding tissue damage. Here we report that Setdb2 was the only protein lysine methyltransferase induced during infection with influenza virus. Setdb2 expression depended on signaling via type I interferons, and Setdb2 repressed expression of the gene encoding the neutrophil attractant CXCL1 and other genes that are targets of the transcription factor NF-kappaB. This coincided with occupancy by Setdb2 at the Cxcl1 promoter, which in the absence of Setdb2 displayed diminished trimethylation of histone H3 Lys9 (H3K9me3). Mice with a hypomorphic gene-trap construct of Setdb2 exhibited increased infiltration of neutrophils during sterile lung inflammation and were less sensitive to bacterial superinfection after infection with influenza virus. This suggested that a Setdb2-mediated regulatory crosstalk between the type I interferons and NF-kappaB pathways represents an important mechanism for virus-induced susceptibility to bacterial superinfection.
in vivo IFNAR-1 blockade
Welten, S. P., et al (2015). "The viral context instructs the redundancy of costimulatory pathways in driving CD8(+) T cell expansion" Elife 4. doi : 10.7554/eLife.07486.
PubMed
Signals delivered by costimulatory molecules are implicated in driving T cell expansion. The requirements for these signals, however, vary from dispensable to essential in different infections. We examined the underlying mechanisms of this differential T cell costimulation dependence and found that the viral context determined the dependence on CD28/B7-mediated costimulation for expansion of naive and memory CD8(+) T cells, indicating that the requirement for costimulatory signals is not imprinted. Notably, related to the high-level costimulatory molecule expression induced by lymphocytic choriomeningitis virus (LCMV), CD28/B7-mediated costimulation was dispensable for accumulation of LCMV-specific CD8(+) T cells because of redundancy with the costimulatory pathways induced by TNF receptor family members (i.e., CD27, OX40, and 4-1BB). Type I IFN signaling in viral-specific CD8(+) T cells is slightly redundant with costimulatory signals. These results highlight that pathogen-specific conditions differentially and uniquely dictate the utilization of costimulatory pathways allowing shaping of effector and memory antigen-specific CD8(+) T cell responses.
in vivo IFNAR-1 blockade
Yang, H., et al (2015). "STAT3 Inhibition Enhances the Therapeutic Efficacy of Immunogenic Chemotherapy by Stimulating Type 1 Interferon Production by Cancer Cells" Cancer Res 75(18): 3812-3822.
PubMed
STAT3 is an oncogenic transcription factor with potent immunosuppressive functions. We found that pharmacologic inhibition of STAT3 or its selective knockout in cancer cells improved the tumor growth-inhibitory efficacy of anthracycline-based chemotherapies. This combined effect of STAT3 inhibition/depletion and anthracyclines was only found in tumors growing on immunocompetent (not in immunodeficient) mice. As compared with Stat3-sufficient control tumors, Stat3(-/-) cancer cells exhibited an increased infiltration by dendritic cells and cytotoxic T lymphocytes after chemotherapy. Anthracyclines are known to induce several stress pathways that enhance the immunogenicity of dying and dead cancer cells, thereby stimulating a dendritic cell-dependent and T lymphocyte-mediated anticancer immune response. Among these therapy-relevant stress pathways, Stat3(-/-) cancer cells manifested one significant improvement, namely an increase in the expression of multiple type-1 interferon-responsive genes, including that of the chemokines Cxcl9 and Cxcl10. This enhanced type-1 interferon response could be suppressed by reintroducing wild-type Stat3 (but not a transactivation-deficient mutant Stat3(Y705F)) into the tumor cells. This maneuver also abolished the improved chemotherapeutic response of Stat3(-/-) cancers. Finally, the neutralization of the common type-1 interferon receptor or that of the chemokine receptor CXCR3 (which binds CXCL9 and CXCL10) abolished the difference in the chemotherapeutic response between Stat3(-/-) and control tumors. Altogether, these results suggest that STAT3 inhibitors may improve the outcome of chemotherapy by enhancing the type-1 interferon response of cancer cells.
in vivo IFNAR-1 blockade
Beug, S. T., et al (2014). "Smac mimetics and innate immune stimuli synergize to promote tumor death" Nat Biotechnol 32(2): 182-190.
PubMed
Smac mimetic compounds (SMC), a class of drugs that sensitize cells to apoptosis by counteracting the activity of inhibitor of apoptosis (IAP) proteins, have proven safe in phase 1 clinical trials in cancer patients. However, because SMCs act by enabling transduction of pro-apoptotic signals, SMC monotherapy may be efficacious only in the subset of patients whose tumors produce large quantities of death-inducing proteins such as inflammatory cytokines. Therefore, we reasoned that SMCs would synergize with agents that stimulate a potent yet safe “cytokine storm.” Here we show that oncolytic viruses and adjuvants such as poly(I:C) and CpG induce bystander death of cancer cells treated with SMCs that is mediated by interferon beta (IFN-beta), tumor necrosis factor alpha (TNF-alpha) and/or TNF-related apoptosis-inducing ligand (TRAIL). This combinatorial treatment resulted in tumor regression and extended survival in two mouse models of cancer. As these and other adjuvants have been proven safe in clinical trials, it may be worthwhile to explore their clinical efficacy in combination with SMCs.
in vivo IFNAR-1 blockade
Calame, D. G., et al (2014). "The C5a anaphylatoxin receptor (C5aR1) protects against Listeria monocytogenes infection by inhibiting type 1 IFN expression" J Immunol 193(10): 5099-5107.
PubMed
Listeria monocytogenes is a major cause of mortality resulting from food poisoning in the United States. In mice, C5 has been genetically linked to host resistance to listeriosis. Despite this genetic association, it remains poorly understood how C5 and its activation products, C5a and C5b, confer host protection to this Gram-positive intracellular bacterium. In this article, we show in a systemic infection model that the major receptor for C5a, C5aR1, is required for a normal robust host immune response against L. monocytogenes. In comparison with wild-type mice, C5aR1(-/-) mice had reduced survival and increased bacterial burden in their livers and spleens. Infected C5aR1(-/-) mice exhibited a dramatic reduction in all major subsets of splenocytes, which was associated with elevated caspase-3 activity and increased TUNEL staining. Because type 1 IFN has been reported to impede the host response to L. monocytogenes through the promotion of splenocyte death, we examined the effect of C5aR1 on type 1 IFN expression in vivo. Indeed, serum levels of IFN-alpha and IFN-beta were significantly elevated in L. monocytogenes-infected C5aR1(-/-) mice. Similarly, the expression of TRAIL, a type 1 IFN target gene and a proapoptotic factor, was elevated in NK cells isolated from infected C5aR1(-/-) mice. Treatment of C5aR1(-/-) mice with a type 1 IFNR blocking Ab resulted in near-complete rescue of L. monocytogenes-induced mortality. Thus, these findings reveal a critical role for C5aR1 in host defense against L. monocytogenes through the suppression of type 1 IFN expression.
in vivo IFNAR-1 blockade
Ma, Y., et al (2014). "Borrelia burgdorferi arthritis-associated locus Bbaa1 regulates Lyme arthritis and K/BxN serum transfer arthritis through intrinsic control of type I IFN production" J Immunol 193(12): 6050-6060.
PubMed
Localized upregulation of type I IFN was previously implicated in development of Borrelia burgdorferi-induced arthritis in C3H mice, and was remarkable due to its absence in the mildly arthritic C57BL/6 (B6) mice. Independently, forward genetics analysis identified a quantitative trait locus on Chr4, termed B. burgdorferi-associated locus 1 (Bbaa1), that regulates Lyme arthritis severity and includes the 15 type I IFN genes. Involvement of Bbaa1 in arthritis development was confirmed in B6 mice congenic for the C3H allele of Bbaa1 (B6.C3-Bbaa1), which developed more severe Lyme arthritis and K/BxN model of rheumatoid arthritis (RA) than did parental B6 mice. Administration of a type I IFN receptor blocking mAb reduced the severity of both Lyme arthritis and RA in B6.C3-Bbaa1 mice, formally linking genetic elements within Bbaa1 to pathological production of type I IFN. Bone marrow-derived macrophages from Bbaa1 congenic mice implicated this locus as a regulator of type I IFN induction and downstream target gene expression. Bbaa1-mediated regulation of IFN-inducible genes was upstream of IFN receptor-dependent amplification; however, the overall magnitude of the response was dependent on autocrine/paracrine responses to IFN-beta. In addition, the Bbaa1 locus modulated the functional phenotype ascribed to bone marrow-derived macrophages: the B6 allele promoted expression of M2 markers, whereas the C3H allele promoted induction of M1 responses. This report identifies a genetic locus physically and functionally linked to type I IFN that contributes to the pathogenesis of both Lyme and RA.
in vivo IFNAR-1 blockade
Stock, A. T., et al (2014). "Type I IFN suppresses Cxcr2 driven neutrophil recruitment into the sensory ganglia during viral infection" J Exp Med 211(5): 751-759.
PubMed
Infection induces the expression of inflammatory chemokines that recruit immune cells to the site of inflammation. Whereas tissues such as the intestine and skin express unique chemokines during homeostasis, whether different tissues express distinct chemokine profiles during inflammation remains unclear. With this in mind, we performed a comprehensive screen of the chemokines expressed by two tissues (skin and sensory ganglia) infected with a common viral pathogen (herpes simplex virus type 1). After infection, the skin and ganglia showed marked differences in their expression of the family of Cxcr2 chemokine ligands. Specifically, Cxcl1/2/3, which in turn controlled neutrophil recruitment, was up-regulated in the skin but absent from the ganglia. Within the ganglia, Cxcl2 expression and subsequent neutrophil recruitment was inhibited by type I interferon (IFN). Using a combination of bone marrow chimeras and intracellular chemokine staining, we show that type I IFN acted by directly suppressing Cxcl2 expression by monocytes, abrogating their ability to recruit neutrophils to the ganglia. Overall, our findings describe a novel role for IFN in the direct, and selective, inhibition of Cxcr2 chemokine ligands, which results in the inhibition of neutrophil recruitment to neuronal tissue.
Product Citations
-
-
Immunology and Microbiology
-
Cardiovascular biology
Cord blood natural killer cell-derived extracellular vesicles inhibit Zika virus infectivity through ITGB2/perforin-mediated envelope disruption in vitro and in vivo.
In Bioact Mater on 1 June 2026 by Cheng, C., Li, R., et al.
PubMed
Zika virus (ZIKV) can traverse the placental barrier, leading to fetal microcephaly and congenital zika syndrome (CZS). The viral E protein mediates host-cell interactions and infection. Here, we demonstrated that cord blood natural killer cell-derived extracellular vesicles (CBNK-EVs) potently inhibit ZIKV infection in vitro without compromising cellular viability. Mechanistically, CBNK-EVs engage ZIKV through ITGB2, a surface-enriched integrin that interacts with the viral E protein, facilitating nanoparticle-virion contact or membrane fusion. This interaction triggers antiviral activity via perforins within extracellular vesicles (EVs), resulting in diminished viral infectivity. Notably, CBNK-EVs not only effectively crossed the placental barrier to protect fetuses from ZIKV-induced pathologies, but also reduced the ZIKV burden in IFN-deficient murine models and decreased CZS incidence and mortality. Additionally, either blockade of ITGB2 with a monoclonal antibody or chelation of Ca2+ with EGTA impaired the anti-ZIKV activity of CBNK-EVs. Collectively, our findings identified CBNK-EVs as natural antiviral nanoparticles that play a pivotal role in curbing ZIKV infection and vertical transmission, offering a promising therapeutic strategy against congenital ZIKV-related complications.
-
-
Ectopic B lymphocyte follicles exacerbate ischemic brain damage via MIF-CD74/CXCR4 and interferon signaling.
In J Clin Invest on 2 March 2026 by Yang, S., Zhang, H., et al.
PubMed
Neuroinflammation, encompassing both innate and adaptive immune responses, plays a crucial role in ischemic stroke. Although B lymphocytes are central to adaptive immunity, their contributions to ischemic stroke remain poorly understood. Here, we demonstrated that B lymphocytes accumulate in ischemic lesions, forming germinal center-like structures at the later stage after stroke, which mainly depended on in situ proliferation. This accumulation correlated with worsened neuroinflammation and ischemic injury, whereas B cell depletion reduced chronic brain damage during stroke. Mechanistically, microglia recruited B cells into ischemic lesions through MIF-CD74/CXCR4 signaling during the early phase of stroke, while IFN-related pathways in B cells further drove neuroinflammation and brain injury. Targeting these pathways markedly alleviated cerebral ischemia and inflammation. Our findings shed light on the role of B lymphocytes in stroke pathology and suggest promising new avenues for therapeutic intervention.
-
-
Cancer Research
-
Immunology and Microbiology
CD38 degrades MAVS through mitophagy to inhibit type I interferon secretion in nasopharyngeal carcinoma cells and impairs CD8+T cell-mediated anti-tumor immunity.
In Nat Commun on 9 February 2026 by Liang, L., Li, W., et al.
PubMed
Activating the type I interferon response in tumor cells and enhancing T cell-mediated anti-tumor immunity have broad clinical applications in tumor immunotherapy. However, the detailed mechanisms underlying the antitumor immune response and type I interferon response in nasopharyngeal carcinoma (NPC) remain unclear and require further elucidation. In this study, we identify CD38 in NPC cells as a key mediator impairing T cell antitumor immunity. Mechanistically, CD38 induces mitochondrial autophagy through PHB2, enhances the interaction between PHB2 and MAVS, leading to the degradation of MAVS protein, and inhibits the type I interferon response and CD8+T cell-mediated anti-tumor immunity. Importantly, CD38 promotes tumor progression and reduces the proportion of CD8+T cells and IFNγ+CD8+T cells in vivo via MAVS. In conclusion, these findings reveal previously unrecognized roles and mechanisms of CD38 in regulating anti-tumor T cell immunity, suggesting that inhibition of CD38 could initiate tumor-targeted immune responses, enhance anti-tumor immunity in patients, and provide new therapeutic strategies for NPC.
-
-
-
Immunology and Microbiology
Lymphotropic Virotherapy Induces DC and High Endothelial Venule Inflammation, Promoting the Antitumor Efficacy of Intratumor Virus Administration.
In Cancer Immunol Res on 3 February 2026 by Ludwig, A. L., McKay, Z. P., et al.
PubMed
Tumor-draining lymph nodes are a pivotal site for antitumor T-cell priming. However, their mechanistic roles in cancer immune surveillance and immunotherapy response remain poorly defined. Intratumor (IT) virotherapy generates antitumor T-cell immunity through multifaceted engagement of innate antiviral inflammation. In this study, we identify type-I interferon (IFNI) signaling in glioma-draining cervical lymph nodes as a mediator of IT polio virotherapy. Transient IFNI signaling after IT administration was rescued by cervical perilymphatic infusion (CPLI) virotherapy, targeting cervical lymph nodes directly. Dual-site (IT plus CPLI) virotherapy induced profound inflammatory reprogramming of cervical lymph nodes, enhanced viral RNA replication and IFNI signaling in dendritic cells and high endothelial venules, augmented antiglioma efficacy in mice, and was associated with T-cell activation in patients with recurrent glioblastoma. A phase II clinical trial of IT plus CPLI polio virotherapy is ongoing (NCT06177964). This study implicates the lymphatic system as a virotherapy target and demonstrates that CPLI virotherapy has the potential to complement brain tumor immunotherapy. See related Spotlight by Kaufman, p. 182.
-
-
-
Cardiovascular biology
-
Immunology and Microbiology
Type I IFN activates border-associated macrophages to drive MHC-I–dependent immune surveillance after stroke
In Research Square on 19 January 2026 by Planas, A., Pedragosa, J., et al.
-
-
-
Cancer Research
-
Genetics
-
Immunology and Microbiology
Nonsense-mediated mRNA decay inhibits TRAF6-dependent anti-tumor immunity in colorectal cancer.
In Cell Rep Med on 16 December 2025 by Wang, Y., Wang, Z., et al.
PubMed
Despite advances in colorectal cancer (CRC) treatment, immunotherapy shows limited efficacy due to low immunogenicity. Nonsense-mediated mRNA decay (NMD) prevents the synthesis of potentially detrimental proteins. While targeting NMD has therapeutic potential, its specific effect on CRC remains uncertain. Our research discovered significant NMD activation and upregulated SMG5 expression in CRC. Inhibition of NMD by small interfering RNA (siRNA) targeting SMG5 or NMD inhibitor NMDI14 remodeled tumor microenvironment (TME) by altering innate immune cells and enhancing CD8+ T cells activation. NMD inhibition also activated TBK1 through upregulation of TRAF6, which was targeted by NMD through its elongated 3'-UTR in a non-canonical manner. High SMG5 and low TRAF6 expression are associated with poor immunotherapy response. Inhibiting NMD enhanced the effectiveness of immune checkpoint blockade (ICB) therapy in CRC. By uncovering the biological relevance and translational potential of targeting NMD to reconstruct TME, this study highlights its promise as a treatment strategy for CRC.
-
-
-
Immunology and Microbiology
-
Cancer Research
Priming with DNMT Inhibitors Potentiates PD-1 Immunotherapy by Triggering Viral Mimicry in Relapsed/Refractory NK/T-cell Lymphoma.
In Cancer Discov on 2 December 2025 by Huang, C., Gao, Y., et al.
PubMed
Anti-PD-1 immunotherapy has demonstrated significant antitumor efficacy in relapsed or refractory NK/T-cell lymphoma (R/R NKTL), but resistance remains a substantial challenge. In this study, we evaluate DNA methyltransferase (DNMT) inhibitors combined with anti-PD-1 mAb in 21 patients with R/R NKTL for whom prior immunotherapy failed. This combination therapy achieved an objective response rate of 66.7% (14/21), with a complete response rate of 47.6% (10/21) and a 2-year overall survival rate of 50.2%. Preclinical models revealed that anti-PD-1 resistance was linked to the absence of CD8+ T-cell infiltration and suppressed IFN pathways. DNMT inhibitors reversed these effects, restoring CD8+ T-cell activities and tumor sensitivity to PD-1 blockade. Mechanistically, DNMT inhibitors triggered DNA demethylation of endogenous retroviral elements, activating viral mimicry via upregulated endogenous nucleic acids and type I IFN signaling. These findings underscore DNMT inhibitors' role in overcoming PD-1 resistance and support their combination with anti-PD-1 as a promising strategy for R/R NKTL.
-
-
-
Immunology and Microbiology
LC3-dependent intercellular transfer of phosphorylated STAT1/2 elicits CXCL9+ macrophages and enhances radiation-induced antitumor immunity.
In J Clin Invest on 1 December 2025 by Li, J. Y., Li, Y. Q., et al.
PubMed
The efficacy of anticancer treatments, including radiotherapy, depends on the activation of type I IFN signaling. However, its regulatory networks and mechanisms remain to be elucidated. Here, we report that tumor cell-intrinsic type I IFN signaling can be transferred to macrophages via secretory autophagy, inducing CXCL9hi macrophages and enhancing CD8+ T cell-mediated antitumor immunity. Mechanistically, K63-linked ubiquitination at the K167 site of phosphorylated STAT2 (p-STAT2) facilitates its binding to LC3B, promoting the loading of p-STAT1 and p-STAT2 into extracellular vesicles and intercellular transference from tumor cells to macrophages, which, however, is suppressed by USP5-mediated STAT2 deubiquitination. Genetic depletion or pharmacological inhibition of USP5 promotes autophagy-dependent unconventional protein secretion of p-STAT1 and p-STAT2, leading to the induction of CXCL9+ macrophages. This process promotes the expression of T cell chemokines and upregulates the antigen presentation machinery, thereby enhancing radiation-induced CD8+ T cell antitumor immunity and radiotherapy efficacy. Our findings reveal a critical role of USP5 in type I IFN-induced antitumor immunity, providing potential targets for improving the efficacy of radiotherapy.
-
-
-
Immunology and Microbiology
-
Cancer Research
Reshaping Tumor-Lymph Node Immune Axis via Targeted Lymphatic Delivery of Dual-Functional Immune Modulator for Enhanced Cancer Immunotherapy.
In ACS Cent Sci on 26 November 2025 by Lim, S. Y., Liu, P., et al.
PubMed
The efficacy of cancer immunotherapy is often limited by the immunosuppressive tumor microenvironment (TME) and insufficient immune activation in tumor-draining lymph nodes (TDLN). Since the TME and TDLN form a dynamic axis crucial for tumor metastasis and resistance to immune checkpoint blockade, strategies that effectively modulate both sites are critical. Here, we present a dissolving microneedle (MN) system that generates nanomicelles (NMCs) for localized delivery of a newly identified dual-functional macrocyclic trichothecene, Roridin E (R.E). R.E induces cancer cell-autonomous secretion of IFN-β and immunogenic cancer cell death (ICD). Direct delivery of R.E to the TDLN via the MN platform reshapes the local immune landscape to suppress cancer while minimizing off-target toxicity. In a B16F10 melanoma model, MN-guided R.E. delivery significantly improved tumor control, reduced lung metastases, and extended overall survival. This approach provides a minimally invasive and effective strategy for integrating natural-product-based therapies with advanced drug delivery systems to target the TME-TDLN axis, thereby improving outcomes in metastatic cancer.
-
-
-
Immunology and Microbiology
Sand fly saliva reprograms skin fibroblasts to enhance arbovirus infection.
In iScience on 21 November 2025 by Keskek Turk, Y., McCafferty-Brown, A., et al.
PubMed
Arbovirus transmission by sand flies is a growing public health concern, yet the early skin events shaping infection outcomes remain undefined. We establish a mouse model of Toscana virus (TOSV) infection that incorporates sand fly salivary factors to mimic natural transmission. Saliva from two distinct sand fly genera significantly enhanced infection and promoted neurological signs and joint inflammation, recapitulating key features of human TOSV disease. In the skin, dermal macrophages and fibroblasts were the main infected cell types, but only fibroblasts generated infectious virus. Saliva reprogrammed fibroblasts into a wound-healing state permissive to viral replication, driving local viral amplification, systemic spread, and thereby clinical disease. These findings identify skin fibroblasts as central determinants of host susceptibility and reveal that sand fly saliva actively remodels the skin to exacerbate viral pathogenesis. This work redefines the skin's role in sand fly-transmitted infection and highlights new targets for therapeutic and vaccine development.
-
-
-
Immunology and Microbiology
Virus envelope glycoprotein targeting bispecific T cell engager protects mice from lethal severe fever with thrombocytopenia virus infection.
In Cell Rep Med on 18 November 2025 by Peng, X., Wang, W., et al.
PubMed
Severe fever with thrombocytopenia syndrome (SFTS) is an emerging hemorrhagic fever disease caused by the SFTS virus (SFTSV). Despite pandemic concerns arising from repeated instances of human-to-human transmission and a high fatality rate, effective anti-SFTSV interventions remain unavailable. Here, utilizing single-cell RNA sequencing (scRNA-seq) and flow cytometry data, we revealed that the deficiency and dysfunction states of T cells, particularly the impaired cytotoxicity and exhausted state of CD4+ T cells, were significantly associated with lethal consequences in SFTS patients. Using an infectious mouse model, we further observed that depletion of CD4+ T and CD8+ T cells was related to elevated viremia and increased fatality rates in SFTSV-infected mice. Accordingly, we designed virus envelope glycoprotein-targeting bispecific T cell engager (BiTE) antibodies to redirect T cells to eliminate SFTSV-infected cells, effectively rescuing mice from lethal SFTSV infection. Collectively, Gn-targeted BiTEs hold potential as a therapeutic option for treating SFTS.
-
-
-
Immunology and Microbiology
-
Genetics
-
COVID-19
-
Cancer Research
SARS-CoV-2 mRNA vaccines sensitize tumours to immune checkpoint blockade.
In Nature on 1 November 2025 by Grippin, A., Marconi, C., et al.
PubMed
Immune checkpoint inhibitors (ICIs) extend survival in many patients with cancer but are ineffective in patients without pre-existing immunity1-9. Although personalized mRNA cancer vaccines sensitize tumours to ICIs by directing immune attacks against preselected antigens, personalized vaccines are limited by complex and time-intensive manufacturing processes10-14. Here we show that mRNA vaccines targeting SARS-CoV-2 also sensitize tumours to ICIs. In preclinical models, SARS-CoV-2 mRNA vaccines led to a substantial increase in type I interferon, enabling innate immune cells to prime CD8+ T cells that target tumour-associated antigens. Concomitant ICI treatment is required for maximal efficacy in immunologically cold tumours, which respond by increasing PD-L1 expression. Similar correlates of vaccination response are found in humans, including increases in type I interferon, myeloid-lymphoid activation in healthy volunteers and PD-L1 expression on tumours. Moreover, receipt of SARS-CoV-2 mRNA vaccines within 100 days of initiating ICI is associated with significantly improved median and three-year overall survival in multiple large retrospective cohorts. This benefit is similar among patients with immunologically cold tumours. Together, these results demonstrate that clinically available mRNA vaccines targeting non-tumour-related antigens are potent immune modulators capable of sensitizing tumours to ICIs.
-
-
-
Immunology and Microbiology
Condensate nanovaccine adjuvants augment CD8+ T-Cell-dependent antitumor immunity through mtDNA leakage-triggered cGAS-STING axis activation.
In Signal Transduct Target Ther on 21 October 2025 by Tang, Y., Luo, Z., et al.
PubMed
The variety and functionality of current clinical vaccine adjuvants remain limited. Conventional aluminum-based adjuvants predominantly induce Th2-biased humoral immunity but exhibit a limited capacity to elicit Th1-mediated cellular immune responses, particularly tumor antigen-specific cytotoxic CD8+ T lymphocytes (CTLs), which are essential for effective cancer vaccine performance. Inspired by natural biomolecular condensates, we developed a versatile noncovalent protein self-assembly strategy distinct from traditional approaches requiring structural domain modifications or bifunctional crosslinkers. Our methodology employs amphiphilic molecules (sodium myristate/SMA and sodium dodecyl thiolate/SDT) as molecular bridges to mediate protein‒protein interactions through hydrophobic forces and disulfide bond formation. This process generates nanoscale protein condensate (PCD) vaccines with exceptional stability. As a novel adjuvant system, these synthetic condensates significantly enhance antigen cross-presentation by optimizing key parameters: antigen loading capacity, lymph node targeting, cytosolic delivery, and lysosomal escape. Consequently, they induce robust antigen-specific CTL responses and humoral immunity, demonstrating potent antitumor efficacy. Importantly, we found that the synthetic protein condensate (PCD) alone can act as a nanoadjuvant. By increasing mitochondrial membrane permeability, PCD induces mitochondrial DNA leakage into the cytosol, activating the cGAS‒STING pathway and promoting DC maturation. This safe and scalable platform eliminates the need for complex covalent modifications or genetic engineering, and it facilitates the design of diverse modular antigens, including neoantigens and viral antigens. Given its straightforward manufacturing process and superior immunogenicity, this synthetic PCD vaccine adjuvant has significant potential for clinical application and translation.
-
-
-
Cancer Research
Super-adjuvant nanoparticles for platform cancer vaccination.
In Cell Rep Med on 21 October 2025 by Kane, G. I., Naylor, T. E., et al.
PubMed
We report on the utility of a "super-adjuvant" nanoparticle (NP) system as a modular, customizable platform for next-generation cancer vaccination. Using nanomaterials engineering technology, we aim to harness not only the effective adjuvanticity of whole-pathogen vaccines, but also the safety of subunit vaccines. Our lipid-based NP platform co-encapsulates agonists of the stimulator of interferon genes (STING) and Toll-like receptor 4 (TLR4) pathways to promote synergistic production of type I interferons and other proinflammatory cytokines in innate antigen-presenting dendritic cells and macrophages. Compared to empty NPs and free agonists, dual-adjuvant NPs administered with antigenic peptides or tumor cell lysate promote increased antigen processing and presentation, drain efficiently to nearby lymph nodes, increase polyfunctional tumor-specific T and B cells, and improve tumor-free outcomes upon vaccination and subsequent challenge with multiple aggressive tumor cells.
-
-
-
Cancer Research
-
Immunology and Microbiology
In situ extended immune activation instantly after tumor resection by oncolytic virus controls postoperative tumor recurrence.
In Cell Rep Med on 21 October 2025 by Guo, C., Gao, T., et al.
PubMed
Postoperative tumor recurrence represents a major challenge for patients. Oncolytic virus (OV) therapy has attracted increasing attention in recent years. Here, we construct a supramolecular hydrogel enabling extended release of type V oncolytic adenovirus (adv), with hydrogel stability confirmed experimentally. In situ treatment with the adv-loaded hydrogel (adv@Nap gel) instantly after tumor resection efficiently activates the type I interferon pathway, induces innate and adaptive immunity, controls postoperative tumor recurrence and metastasis, and prolongs mouse survival. We verify the ability of instant in situ treatment with adv@Nap gel to inhibit postoperative tumor recurrence. Notably, oncolytic herpes simplex virus or vaccinia virus loaded in Nap gel can also control postoperative tumor recurrence. Thus, hydrogel-loaded OVs that induce extended immune activation represent a paradigm for sustained antitumor immunotherapy, and in situ sustained immune activation initiated during surgery may represent an important and universal treatment guideline.
-
-
-
Immunology and Microbiology
EP300 compromises antitumor immunity by increasing SOCS1 expression.
In J Immunother Cancer on 15 October 2025 by Zeng, Y., Zhou, Y., et al.
PubMed
Beyond supporting cancer cell proliferation, tumor growth relies on the ability of cancer cells to evade immune surveillance. Identifying novel molecules that promote tumor immune escape may help develop more effective immunotherapeutic strategies. The histone acetyltransferase E1A-binding protein p300 (EP300) is a key epigenetic regulator that modulates gene transcription through chromatin remodeling and acetylation of histones and transcription factors. However, its role in regulating immune evasion remains incompletely understood. This study investigates the impact of EP300 on tumor immune escape and suggests its potential as an immunotherapeutic target.
-
-
Macrophages orchestrate elimination of Shigella from the intestinal epithelial cell niche via TLR-induced IL-12 and IFN-γ.
In Cell Host Microbe on 10 September 2025 by Eislmayr, K. D., Nichols, C. A., et al.
PubMed
Bacteria of the genus Shigella replicate in intestinal epithelial cells and cause shigellosis, a severe diarrheal disease that resolves spontaneously in most healthy individuals. During shigellosis, neutrophils are abundantly recruited to the gut and have long been thought to be central to Shigella control and pathogenesis. However, how shigellosis resolves remains poorly understood due to the longstanding lack of a tractable and physiological animal model. Here, using our newly developed Nlrc4-/-Casp11-/- mouse model of shigellosis, we unexpectedly find no major role for neutrophils in limiting Shigella or in disease pathogenesis. Instead, we uncover an essential role for macrophages in the host control of Shigella. Macrophages respond to Shigella via Toll-like receptors (TLRs) to produce IL-12, which then induces IFN-γ, a cytokine that is essential to control Shigella replication in intestinal epithelial cells. Collectively, our findings reshape our understanding of the innate immune response to Shigella.
-
-
Immunology and Microbiology
Oropouche virus disrupts neurodevelopment and is vertically transmitted
In Research Square on 9 September 2025 by Jurado, K., Bannerman, C., et al.
-
-
Chronic social defeat stress induces meningeal neutrophilia via type I interferon signaling in male mice.
In Nat Commun on 1 September 2025 by Kigar, S. L., Lynall, M. E., et al.
PubMed
Inflammation is increasingly recognized as a risk factor for psychiatric disorders. Animal models of stress and stress-related disorders are associated with blood neutrophilia. The mechanistic relevance of this to symptoms or behavior is unclear. We characterized the immune response to chronic social defeat (CSD) stress at brain border regions in male mice. Here we show that chronic, but not acute, stress causes neutrophil accumulation in the meninges-i.e., "meningeal neutrophilia"- but not the brain. CSD promotes neutrophil trafficking to meninges via vascular channels originating from skull bone marrow (BM). Transcriptional analysis suggests CSD increases type I interferon (IFN-I) signaling in meningeal neutrophils. Blocking this pathway via the IFN-I receptor (IFNAR) protects against the negative behavioral effects of CSD stress. Our identification of IFN-I signaling as a putative mediator of meningeal neutrophil recruitment may facilitlate development of new therapies for stress-related disorders.
-
-
Immunology and Microbiology
Engineered bacteria launch and control an oncolytic virus.
In Nat Biomed Eng on 15 August 2025 by Singer, Z. S., Pabon, J., et al.
PubMed
The ability of bacteria and viruses to selectively replicate in tumours has led to synthetic engineering of new microbial therapies. Here we design a cooperative strategy whereby Salmonella typhimurium bacteria transcribe and deliver the Senecavirus A RNA genome inside host cells, launching a potent oncolytic viral infection. 'Encapsidated' by bacteria, the viral genome can further bypass circulating antiviral antibodies to reach the tumour and initiate replication and spread within immune mice. Finally, we engineer the virus to require a bacterially delivered protease to achieve virion maturation, demonstrating bacterial control over the virus. Together, we refer to this platform as 'CAPPSID' for Coordinated Activity of Prokaryote and Picornavirus for Safe Intracellular Delivery. This work extends bacterially delivered therapeutics to viral genomes, and shows how a consortium of microbes can achieve a cooperative aim.
-